Treatment Consultants Who Help Families Navigate Recovery

Table of Contents
Related BlogsWhy Families Engage Treatment Consultants
The Treatment Gap and Family Burden
The treatment gap—defined as the difference between those needing specialty substance use or mental health treatment and those actually receiving it—remains substantial. According to the 2024 National Survey on Drug Use and Health, 89% of individuals with substance use disorders did not access specialty treatment in the past year, despite rising awareness and available interventions1. This leaves families carrying much of the burden: managing crises, seeking solutions, and trying to coordinate fragmented care systems without adequate support.
Checklist: Signs of the Treatment Gap and Family Burden
- Loved one has a diagnosed or suspected substance use or mental health disorder.
- Difficulty accessing or navigating specialty treatment providers.
- Recurring crises or hospitalizations without lasting stability.
- Family members experiencing caregiver burnout, anxiety, or confusion.
- Repeated failed attempts to coordinate care independently.
Research consistently shows that family members often act as the primary support system but frequently lack the training and resources needed to facilitate recovery effectively3. The pressures can lead to emotional exhaustion, strained relationships, and missed opportunities for timely intervention. For affluent families, complexity increases with private pay options, out-of-network providers, and the need for customized, confidential care.
Treatment consultants offer crucial guidance by helping families bridge the gap between clinical needs and available resources. This approach works best when families face repeated barriers, high emotional distress, or escalating crises that threaten safety and stability. Evidence suggests that engaging professional support increases treatment engagement by up to 50% and improves long-term outcomes for both individuals and their support networks4.
When Internal Resources Reach Limits
Families often bring deep commitment and resilience to supporting a loved one’s recovery. However, even affluent families with substantial means encounter limits—especially when private-pay options, complex diagnoses, and confidentiality requirements strain personal bandwidth. Symptoms of resource exhaustion include disrupted routines, chronic stress, and decision fatigue. In high-net-worth households, demands may also include managing household staff or coordinating multiple providers across states or internationally.
Decision Tool: Signs That Family Resources Are Maxed Out
- Persistent escalation of crises, despite family efforts.
- Family members cancelling work or travel to respond to emergencies.
- Difficulty maintaining boundaries or consistent support.
- Repeatedly unclear on next steps or feeling pressured to make high-stakes clinical decisions.
- Sense of isolation even with access to private resources.
Research underscores that when families reach these limits, self-directed management can unintentionally worsen burnout and lead to missed opportunities for early intervention3. Treatment consultants provide a structured, evidence-based process to relieve pressure and restore clarity.
This path makes sense for families experiencing ongoing instability or feeling overwhelmed by clinical, legal, and logistical complexity. Licensed consultants use multidisciplinary assessment and care-planning methods shown to improve treatment engagement by 30-50% compared to individual-only approaches4.
Comprehensive Assessment by Treatment Consultants
Multidimensional Clinical Evaluation
A multidimensional clinical evaluation forms the backbone of effective recovery planning. Treatment consultants conduct assessments that reach beyond surface-level diagnoses, drawing on established frameworks such as the American Society of Addiction Medicine (ASAM) Criteria. This multidimensional lens is crucial for affluent families facing complex presentations, such as dual diagnoses or international care coordination.
Clinical Evaluation Framework: Key Domains
| Assessment Domain | Focus Area |
|---|---|
| Medical & Psychiatric | History of co-occurring conditions, medication review, and physical health status. |
| Substance Use | Patterns of use, tolerance levels, and immediate withdrawal risks. |
| Functional Status | Emotional, cognitive, and behavioral functioning in daily life. |
| Systemic Factors | Family dynamics, support structures, and readiness for change. |
| Environmental | Social, educational, legal factors, and recovery resources. |
A thorough evaluation typically requires a multidisciplinary team: licensed clinicians, medical doctors, and sometimes educational or legal consultants. Time investment varies but may range from several hours to multi-day processes, especially when synthesizing records, conducting interviews, and collaborating with outside providers. For families managing multiple obligations or privacy concerns, this approach ensures the resulting plan is both clinically sound and practical.
Consider this method if your client’s case involves recurring crises, failed prior treatments, or unresolved diagnostic questions. Research shows that comprehensive, team-based assessment improves the accuracy of treatment recommendations and long-term outcomes for both individuals and their families4.
Diagnostic Questions for Family Readiness
Treatment consultants use structured diagnostic questions to uncover not just the clinical status of the individual in crisis, but also the readiness and capacity of the family system. This process extends beyond surface agreement, probing for hidden resistance, unspoken fears, and prior unsuccessful attempts at coordination.

Evidence shows that families who complete readiness assessments are more likely to engage in treatment consistently, with improved adherence rates and lower drop-off during transitions between care settings4.
Readiness Assessment Tool: Core Diagnostic Questions
- Are all key family members aligned on the need for intervention or treatment?
- What prior efforts have been made, and what barriers led to limited success?
- How willing is the family to accept professional guidance on boundaries, communication, and next steps?
- Is there clarity about financial commitment, privacy concerns, and expectations for outcomes?
- Has stigma or fear of disclosure delayed seeking specialized help?
- Are cultural, legal, or logistical complexities (e.g., multiple residences, international travel) present?
This approach is ideal for families who have experienced repeated setbacks, or where multiple decision-makers are involved and not all are equally committed to the recovery process. The assessment phase can be conducted through joint interviews, individual conversations, or digital surveys, depending on privacy needs and family dynamics. Time investment ranges from 2–6 hours, and may involve multiple sessions to reach consensus and clarify expectations.
Clarity and Coordination When Life Gets Complex
For 30 years, Feinberg Consulting has provided concierge-level intervention, advocacy, consulting, and care coordination for behavioral health challenges, catastrophic injuries, complex medical conditions, and senior care.
Our independent clinical team partners with families and professionals to clarify next steps, coordinate trusted resources, and bring steady guidance when situations feel overwhelming.
Coordinating Multi-System Care Plans
Building Independent Provider Networks
For affluent families navigating multi-system recovery, the ability to construct an independent provider network is critical. Treatment consultants use rigorous vetting protocols, drawing on direct experience and established standards to ensure each provider meets the unique needs of the household. This solution fits families prioritizing privacy, seeking out-of-network options, or facing rare diagnoses where mainstream programs may not suffice.
Unlike referral lists generated by in-network insurance relationships, independently built networks emphasize neutrality and quality. Consultants invest substantial time (often 5–15 hours per case) into background checks, reference calls, and coordinating intake processes.
Provider Vetting Checklist: Building an Independent Network
- Confirm provider licensure and relevant clinical credentials.
- Assess experience with complex, affluent family cases.
- Ensure alignment with client privacy and confidentiality needs.
- Review outcomes data and references from similar cases.
- Evaluate readiness for multidisciplinary collaboration.
The process typically includes reviewing providers’ outcome data, confirming their willingness to collaborate, and ensuring no financial ties compromise their recommendations7. Evidence shows that independent, multidisciplinary care coordination reduces emergency interventions and improves long-term treatment engagement by 30–50% compared to fragmented, provider-driven models4.
Integration Across Medical and Behavioral
Effective integration of medical and behavioral health domains is essential for families managing complex recovery journeys. Treatment consultants play an instrumental role by bridging gaps between psychiatrists, therapists, primary care, and specialty providers. This integration is especially crucial when co-occurring diagnoses, such as substance use disorder and a chronic medical condition, increase the risk of fragmented care or conflicting recommendations.
Integration Checklist: Ensuring Seamless Care
- Establish shared communication protocols among all clinicians.
- Align treatment goals between medical and behavioral health providers.
- Implement regular interdisciplinary case reviews.
- Confirm medication management is coordinated with therapy and other supports.
- Track outcomes and adjust plans collaboratively.
This method works when families require precise alignment of medication management with behavioral therapies, especially where privacy or multiple locations add complexity. Treatment consultants typically facilitate biweekly or monthly multidisciplinary meetings, manage secure information sharing, and develop unified care plans. The time investment can range from 4–10 hours per month, depending on the number of providers and the intensity of coordination needed.
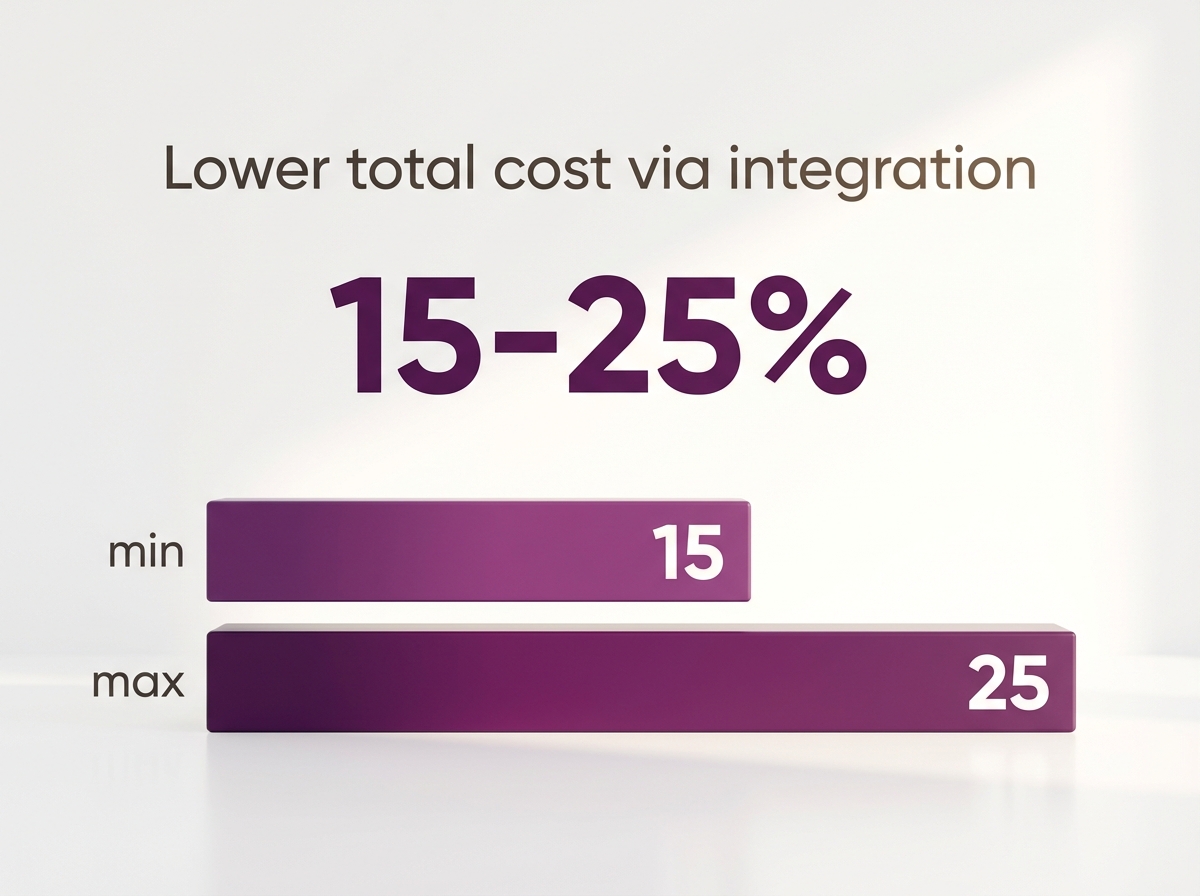
Integrated care models have been shown to reduce emergency department visits by 15–25% and improve treatment adherence and satisfaction in complex cases5. By ensuring that all providers operate from a single, evolving plan, consultants help prevent miscommunication and support sustained recovery.
Implementation and Ongoing Management
Crisis Response and Treatment Transport
When acute behavioral health or substance use crises occur, treatment consultants provide a stabilizing presence and orchestrate time-sensitive interventions. Their expertise extends to coordinating safe transport—whether to inpatient treatment, psychiatric stabilization, or medical detox—especially in situations where commercial travel is unsafe or discretion is paramount.
Crisis Response and Transport Protocol
- Pre-identify emergency contacts and preferred medical facilities.
- Establish rapid-response protocols with all care team members.
- Secure safe, private transport options for urgent admissions.
- Prepare necessary documentation (medical records, consent forms, insurance info).
- Arrange for clinical staff or companion to accompany during high-risk transfers.
Research demonstrates that professional involvement during crisis events can reduce inappropriate hospitalizations and emergency interventions, ensuring individuals receive care at the right level and setting3. Consultants commonly allocate 2–8 hours per crisis event, often mobilizing within hours to provide on-site support, facilitate de-escalation, and coordinate with local providers.
Opt for this framework when clinical, legal, or logistical complications make self-directed crisis management unsustainable. The resource commitment may also include partnering with private medical transport or sober companion services, depending on acuity and geography.
Monitoring Progress and Adjusting Plans
Effective recovery management is grounded in proactive monitoring and agile adjustment. Treatment consultants typically implement a structured review process, using both quantitative (e.g., attendance rates, symptom scales) and qualitative (e.g., family feedback, observed behavior changes) measures. These reviews may be conducted via weekly team calls or secure digital dashboards, requiring a time investment of 2–4 hours per week from the clinical team, plus periodic family consultations.

Progress Monitoring Checklist: Key Metrics
- Weekly review of clinical goals and progress across all providers.
- Regular updates on medication adherence, attendance, and engagement in therapy.
- Tracking relapse warning signs or shifts in motivation.
- Ongoing communication with family to assess support needs and dynamics.
- Quarterly outcome reviews and plan adjustments based on objective data.
Prioritize this when families seek to minimize regression and maximize long-term success. Consultants use evidence-based tools to identify early signs of relapse or disengagement, allowing for swift intervention. Data shows that ongoing case monitoring and responsive plan adaptation can increase treatment retention by up to 50% and reduce emergency incidents4.
Your Next 30 Days: Building Recovery Infrastructure
The first 30 days determine whether clinical recommendations translate into sustainable outcomes. For families navigating addiction or mental health crises, this window requires more than a treatment plan on paper. It demands an independent clinical team to manage implementation, coordinate providers, and adjust course as real-world challenges emerge. The infrastructure built during this period either supports long-term stability or creates gaps that lead to relapse and renewed crisis.
Building effective recovery infrastructure means addressing practical needs alongside clinical care. This includes coordinating medical appointments, establishing therapeutic routines, managing medication protocols when appropriate, and creating safety plans for potential setbacks. Families often find that organizing documentation, centralizing communication channels, and designating decision-makers streamlines the process significantly.
The next 30 days also provide an opportunity to assess what's working and adjust what isn't. Clinicians can refine treatment recommendations based on real-world implementation, address emerging challenges proactively, and ensure all providers are aligned on the care plan. This period requires patience and flexibility as individuals adjust to new routines and families adapt to their evolving roles.
Establishing these systems early creates momentum that carries through subsequent phases of recovery, reducing crisis moments and building confidence in the overall approach.
Frequently Asked Questions
What credentials should clinical consultants hold for complex addiction and mental health cases?
For complex addiction and mental health cases, clinical consultants should hold advanced behavioral health licenses such as LMSW (Licensed Master Social Worker), LMHC (Licensed Mental Health Counselor), or equivalent state-level clinical credentials. Board certification or specialty training in addiction, co-occurring disorders, or family systems approaches further strengthens expertise. Evidence-based practice standards recommend consultants have multidisciplinary experience and demonstrated proficiency in assessment, treatment planning, and care coordination for high-acuity cases 28. This path makes sense for families dealing with multi-layered diagnoses, private-pay settings, or cases where confidentiality and cross-system navigation are priorities. Treatment consultants with these qualifications offer the rigor and professional grounding needed to manage high-risk, high-need situations effectively.
How do private-pay clinical consulting fees compare to potential cost savings from coordinated care?
Private-pay clinical consulting fees often represent a significant upfront investment for families, but coordinated care led by treatment consultants has been shown to generate measurable cost savings over time. Integrated care management can reduce total costs by 15–25% in complex behavioral health cases by minimizing emergency department visits, unnecessary hospitalizations, and redundant services 5. Structured case management programs deliver a return on investment (ROI) of three to five times the consulting fee by improving outcomes and reducing high-cost crises 9. For families juggling multiple providers or out-of-network care, the financial impact of well-coordinated planning and monitoring frequently outweighs the initial consulting expense.
How long does comprehensive assessment typically take before treatment recommendations are finalized?
A comprehensive assessment conducted by treatment consultants usually requires a time investment of 6 to 18 hours spread over several days. This period includes intake interviews, record review, family meetings, and multidisciplinary team discussions. For cases with complex medical, psychiatric, or legal factors, the process can extend to one or two weeks to ensure all relevant data is synthesized and every stakeholder is consulted. Such diligence is especially important for affluent families managing privacy or logistical challenges. Most recommendations are finalized within 7 to 14 days, though urgent cases may be expedited. This timeline aligns with standards outlined by the American Society of Addiction Medicine and recent peer-reviewed research 24.
What distinguishes independent clinical consultants from provider-affiliated care coordinators?
Independent clinical consultants operate without financial ties to treatment facilities, maintaining neutrality when assessing options and making recommendations. In contrast, provider-affiliated care coordinators are typically employed by or contracted with a specific program or hospital, which can create pressure to keep referrals within that network. This distinction is crucial for affluent families seeking impartial guidance; independent treatment consultants prioritize individual clinical needs, privacy, and long-term outcomes rather than organizational quotas. Evidence-based standards highlight that independent consultants are more likely to vet providers thoroughly and build customized, multidisciplinary networks that minimize bias 7. This model supports truly client-centered recovery planning.
How do families evaluate whether a consultant's provider network aligns with clinical needs versus convenience?
Families can evaluate a consultant’s provider network by examining both the thoroughness of the vetting process and the relevance of recommended professionals to the client’s specific clinical needs. Look for evidence that treatment consultants have reviewed provider licensure, outcome data, and experience with similar complex cases, rather than relying on geographic proximity or longstanding relationships alone 7. Ask for clear documentation of how each provider was selected and whether multidisciplinary collaboration and privacy standards are prioritized. This approach works best when consultants demonstrate transparency and provide references from other families with similar profiles. Families should prioritize networks tailored to clinical complexity, not just logistical convenience, to maximize long-term recovery outcomes.
What measurable outcomes indicate effective care coordination in the first 90 days?
Measurable outcomes in the first 90 days of effective care coordination include reductions in crisis events or emergency department visits, consistent attendance at therapy and medical appointments, and improved medication adherence. Families commonly observe enhanced communication among providers and a clear, unified treatment plan. Early warning signs of relapse or disengagement are identified and addressed quickly, minimizing regression. Research indicates that treatment consultants who monitor these metrics achieve a 30-50% increase in treatment engagement and a 15-25% reduction in emergency interventions during the initial phase of coordinated care 45. These benchmarks help families gauge whether the consulting approach is supporting safety, stability, and progress.
When should families transition from intensive consulting support to maintenance-level coordination?
Transitioning from intensive consulting support to maintenance-level coordination is appropriate when a family demonstrates sustained stability, reduced crisis frequency, consistent engagement in treatment, and strong communication among all providers. Treatment consultants typically recommend this shift once measurable outcomes—such as decreased emergency interventions and improved adherence—are achieved for at least 60 to 90 days 45. Maintenance-level coordination focuses on periodic check-ins, outcome tracking, and timely adjustment of care plans, rather than daily oversight. This approach suits families whose needs have shifted from crisis management to long-term support, allowing autonomy while still providing professional guidance for evolving situations.
References
- 2024 National Survey on Drug Use and Health (NSDUH): Main Findings. https://www.samhsa.gov/data/sites/default/files/reports/rpt39443/2024-nsduh-results.pdf
- American Society of Addiction Medicine (ASAM) Criteria and Treatment Standards. https://www.asam.org/standards-and-guidelines
- National Alliance on Mental Illness (NAMI): Family Support Policy and Research. https://www.nami.org/advocacy/policy-priorities/family-support-and-peer-support
- PubMed: Peer-Reviewed Research on Family-Based Treatment and Case Management. https://pubmed.ncbi.nlm.nih.gov/
- Centers for Medicare & Medicaid Services (CMS) Data on Behavioral Health Service Utilization and Outcomes. https://www.cms.gov/research-statistics-data-systems/research-statistics-data-and-systems
- National Institute on Drug Abuse (NIDA): Principles of Drug Addiction Treatment. https://nida.nih.gov/publications/principles-drug-addiction-treatment-research-based-guide-third-edition/evidence-based-approaches-drug-addiction
- The Joint Commission: Quality Standards for Behavioral Health and Case Management. https://www.jointcommission.org/standards/
- American Psychological Association: Standards for Evidence-Based Practice and Treatment Planning. https://www.apa.org/science/standards/treatment
- American Case Management Association (ACMA): Case Management Standards and Research. https://www.acmweb.org/
- NIH: Family Systems and Addiction Recovery - Meta-Analysis of Intervention Effectiveness. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4838507/
When the Path Forward Isn’t Clear
Families often reach out when addiction, mental health concerns, medical crises, or aging-related challenges begin to affect daily life. Feinberg Consulting offers concierge-level intervention, advocacy, consulting, and care coordination to help families understand their options and move forward with confidence. Through careful assessment, trusted recommendations, and coordinated support, we help families bring structure, clarity, and stability to complex situations.
Related Blogs

Dear Parents: What I Really Need When I Come Home for the Summer
Finally, summer break! After a year of surviving endless assignments and late-night study sessions, I’m back home. At first, it felt amazing—no more deadlines, no more dorm chaos. But as the days...

Busted Brackets & Broken Bankrolls: The Rise of College Gambling During March Madness
By Steve Feldman, CEO Each year, as March Madness kicks off, millions of Americans turn their attention to the NCAA tournament...

Empowering Families, Coordinating Care: Navigating Dementia and Aging with Compassion and Expertise
As we age, our needs change. For some, this means a gradual slowing down, while for others, it means navigating the challenges of dementia and other complex health conditions.
.webp)
%20(1).avif)






